LASIK Eye Center in San Jose

More than 11 million Americans have common vision problems like nearsightedness, farsightedness, and astigmatism. These conditions are the most common cause of correctable visual impairment. Many people turn to glasses and contact lenses to correct these problems.
However, if you’re looking for a permanent solution, LASIK is the way to go. We proudly serve the greater San Francisco areas with premier LASIK procedures, schedule your consultation today!
What is LASIK?
LASIK surgery is a common surgical procedure that permanently corrects refractive errors. Those who are sick of their glasses and contact lenses typically seek out LASIK surgery as an alternative.
When a person has a refractive error, it means that their eye is misshapen. Irregular cornea shape means that light cannot refract properly onto the retina, resulting in blurry vision. LASIK surgery aims to reshape the cornea to allow proper light refraction.
The Benefits
There are many benefits to LASIK, some of which include fast visual recovery, limited if any discomfort, and a lowered risk of glare and halos compared to older procedures such as radial keratotomy (RK). New developments in LASIK, especially custom wavefront LASIK, have been perfected to further reduce the risk of glare and halo. Most patients are very happy with the results.
It’s no wonder that LASIK laser vision correction has quickly emerged as one of the true medical breakthroughs of modern history. LASIK, the most widely used form of laser vision correction, is the fastest-growing type of refractive surgery. It is very versatile and can treat both nearsightedness and farsightedness with or without astigmatism.
Over 98% of people who have LASIK achieve somewhere between 20/20 and 20/40 vision without glasses or contact lenses and we proudly offer this procedure to our patients throughout the San Jose and San Francisco area.
Am I a Candidate?
LASIK surgery is not for everyone. You may not be able to undergo LASIK surgery if you:
- Are under the age of 18
- Are pregnant or nursing
- Are diabetic, or living with another autoimmune disease
- Have had a previous eye injury
- Have had other types of eye surgery
- Have a chronic dry eye disease
- Have thin, unstable corneas (usually as a result of keratoconus)
The only way to know for sure if you are a candidate for LASIK surgery is to come in for a LASIK consultation at Ellis Eye. If you live in the San Francisco and San Jose areas and want to start the process now? Take our 2-minute online self-evaluation to see if you’re a likely candidate for LASIK!
Your LASIK “Prescription” – As Unique As Your DNA!
At Your Consultation
If you have not already done so at a screening evaluation, a complete medical and eye history will be taken. This will include a review of your health and medical conditions, medications you are taking, allergies as well as a discussion of your ocular health and status including your vision correction history.
It will be necessary for you to communicate any medical or eye conditions or diseases that have been diagnosed or treated among your family members.
First, a technician will begin taking a number of measurements. These will include your visual acuity with and without your current method of vision correction, whether that is glasses or contacts. A digital map of your corneal shape – called corneal topography – will be taken. A measurement of your pupils will be performed as detailed later.
In order to get final measurements of the prescription, your prescription will be measured both in its natural state and after having drops placed in your eyes. A test will be performed to see which eye is your dominant eye, and most importantly, the thickness of your cornea will be measured to make sure that there is enough corneal tissue present to allow LASIK to be performed.
Additional testing including your intraocular pressure will be conducted and observations will be made of the health of your cornea, lens, and tear film using an instrument called a slit lamp. This is actually a microscope through which living tissue can be carefully examined.
After the drops have had their full effect, the doctor will examine the health of your retina and optic nerves in order to give your eyes a “clean bill of health” for LASIK.
What to Expect During Your LASIK Surgery Process
When you arrive at the practice on your day of surgery, you should expect to have the staff begin to both prepare you for your treatment and to make you comfortable. If you have taken our online LASIK self-evaluation test and are curious to speak with a member of our staff about LASIK, congratulations – you’re one step closer to clear vision! Your next step is your LASIK evaluation.
Here is a breakdown of what to expect during your LASIK evaluation with Ellis Eye & Laser Medical Center.
1. Eye Testing
A dilated examination allows us to most accurately ascertain your refractive errors and facilitates the visualization of the tissues and structures within the eye. You will be examined for cataract and diseases of the retina. The retina is composed of the photoreceptors which detect the light in the image focused upon them.
We will also examine your cornea – The outermost surface of the eye, through which you see, and is the principal refracting surface of the eye. The status of the tear film layer which covers the surface of the cornea is important to ocular health. If dry eye is present due to insufficient tear production, artificial tear drops, punctum plugs, or Restasis eye drops may be prescribed.
In addition, several sophisticated scientific scans of the visual system will be performed:
- EyeSys Corneal Topography. A topographical map will be constructed of the front surface of the cornea by shining multiple placebo disk mires on the cornea. A mathematical analysis of the spacing between mires will be used by the computer to draw a three-dimensional picture of your cornea.
- Goldman Tonometry will be evaluated to determine the intraocular pressure within your eyes to rule out glaucoma.
- An Orbscan of the cornea will measure the curvatures of both the front and back surfaces of the cornea and will also measure the thickness of your cornea. Candidates for LASIK must have enough tissue for the LASIK procedure. If there is insufficient corneal tissue present for your degree of myopia or astigmatism, PRK or Advanced Surface Ablation may be the procedure of choice.
- The Zywave Aberrometer will be used to measure the wavefront pattern of the refractive media of your eyes. Specifically, the Aberrometer will detect higher-order optical aberrations that degrade the quality of vision especially at night, and can be responsible for glare and halos in the vision. Thanks to modern technology Zyoptix laser vision correction can reduce or eliminate these higher-order visual distortions, and in some cases improve the vision beyond 20/20.
You will be asked to sit and recline on a comfortable bed-like chair or platform and some additional numbing drops will be placed in your eyes. The surgeon or staff will clean the area around your eye by using a small sterile pad and some liquid to gently scrub your eyelids and adjacent areas.
2. Arrangements Before Surgery
- Contact lens wear should be stopped at least 3 days prior to surgery if soft lenses have been worn and longer for hard lenses or semipermeable lenses.
- Please arrange for transportation home on the day of surgery as you should not drive home yourself.
- Most LASIK patients are able to drive themselves the following day for the one-day post-operative visit, but only if you feel that your vision is okay.
- Following the EpiLasik and PRK procedures, you will not be able to drive for at least 5 days. At the time of your postoperative visits, your doctor will advise you when healing has been sufficient to allow you to drive.
- Please arrange for time off from work for your procedure. Our doctors will be happy to provide medical excuses for your employer if necessary.
- Do not wear eye makeup on the day of surgery. Particles of mascara can lodge under the LASIK flap.
- Do not use perfumes or aftershave lotions on the day of surgery. Vapors from these can interfere with the laser beam and be harmful to the optics of the laser.
- There are usually no restrictions on eating or taking medications on the day of surgery, but please advise us as to any medicines you are taking.
Postoperative visits are usually on the first day following surgery, 1-week post-op, 1-month post-op, and the second or third month as well.
3. The Day of the LASIK Procedure
In order to ensure a semi-sterile environment, you will put on a surgical gown prior to entering the laser room. The nurse will take your vital signs and enter them into your surgical chart.
Prior to the procedure, your ophthalmologist will spend time with you to go over your proposed treatment and to answer any further questions that you may have. When you are ready, you will be given an oral tablet such as Valium to relax you.
You will be taken into the laser room and lie down on a flatbed under the laser. The area around your eyes will be washed with an alcohol sponge and a sterile towel will be used to drape off the periocular area. Numbing drops will be placed in the eye and a small eyelid speculum will be positioned to hold the lids open.
It is important not to squeeze the eyelids over the speculum since oil from the eyelash follicles can be released and can cause post-operative inflammation.
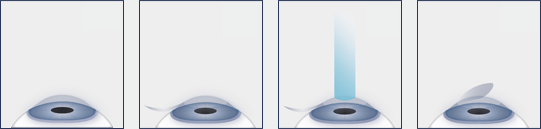
Relax, and open both eyes. There will be no pain or discomfort with the procedure. At the appropriate time, the microkeratome will be placed to create the LASIK flap. There will be pressure, but no pain. The vision in the eye will be gone for a second or two and then will return when the device is removed. It will take about 5 to 10 seconds to make the flap.
The eye surgeon will fold the flap back and the excimer laser will be used to perform the optical correction. Be sure to keep both eyes open and look at the red aiming beam under the laser. After the treatment is finished, the surgeon will reposition and dry the flap with oxygen. The lid speculum will be removed and you will follow the nurse to the post-op area where your eye surgeon will again examine the eyes.
You will be sent home with your medications, which will include antibiotic and anti-inflammatory drops, and sleeping and pain pills. Although there is no pain during the laser procedure after the topical anesthetic drops wear off there will be mild discomfort with the LASIK procedure for the first post-op day. Be careful not to rub your eyes and do not put any pressure on them or sleep on them on the first day.
You will be awake and able to communicate for this very brief procedure. It lasts about 15-30 seconds. A delicate instrument, called a microkeratome, is used to create a very thin flap of corneal tissue. Once this tissue flap is created, the surgeon positions the laser beam over the eye, directing light pulses to achieve the desired correction. The flap is carefully placed back in its original position. Because of the anatomy of the cornea, no stitches will be necessary.
You will be given eye drops to help the eye to heal and to alleviate dryness. Healing time is minimal and after two or so hours of rest, the results will be apparent. For some patients, recovery may take longer.
4. Post-Operative Care and Recovery
Your first postoperative visit will be mandatory on the first post-op day. LASIK patients generally see well enough to drive to the office, however, if your vision is still blurred do not drive. Usually, it will clear in 1-2 days, but it can sometimes take longer. You will use antibiotic and corticosteroid anti-inflammatory drops for several days or weeks.
Generally, the antibiotic is stopped after the first day, and anti-inflammatory drops after several weeks. the ophthalmologist will change your medications as needed.
Patient Financing
Your patient counselor will find the very best financing and payment plan for your specific needs. We work closely with many sources of patient financing such as CareCredit and can tailor specific programs, including those with delayed payments, so that refractive eye surgery will be affordable and within your ability to pay.
A small deposit will be required when you schedule your procedure in order to hold your place. Your surgery must be fully paid for by the day of surgery or alternatively, your financing plan must have been approved.
LASIK Alternatives
Certain ocular conditions may rule against your being a good refractive surgery candidate. These include:
- Eye infections or inflammations
- Dry eye conditions unresponsive to treatment
- Thin or scarred corneas including Keratoconus
- Active rheumatologic conditions such as lupus in a flare-up and not in remission
- Degenerative conditions of the cornea
- Use of certain drugs
- Uncontrolled diabetes mellitus.
- Certain time intervals during pregnancy.
Your patient counselor will confer with our doctors and determine if you are a candidate for LASIK or other refractive procedures. The counselor will also assist you in determining the best procedure for you. She will explain the pros and cons of each procedure, as well as the risks and complications.
Your surgeon is not required to explain risks that are extremely remote or those that become known at a later time.
Your surgeon will provide you with information, such as pamphlets and research, that can help you to decide whether or not to undergo the procedure. Your patient counselor and other staff members are also available for any additional questions. Your counselor will tell you what to expect on the day of surgery, and about the postoperative recovery course. She will tell you about medications you will need to take and help to call in any prescriptions to your pharmacist.
To schedule your FREE laser vision correction evaluation call Ellis Eye and Laser Medical Center at 1-800-SEE-SHARP (1-800-733-7427). Our clinics are located in San Francisco, San Jose, Walnut Creek, El Cerrito, Roseville, Gilroy, and Corte Madera, California.

